How to Read a 12-Lead ECG Step by Step
For medical students and junior doctors
Meta description: Learn how to read a 12-lead ECG step by step using a practical approach for medical students and junior doctors. Understand rate, rhythm, axis, intervals, ST segments, and T waves.
Quick Answer
To read a 12-lead ECG step by step, start by checking the patient details, calibration, and paper speed, then assess rate, rhythm, axis, P waves, PR interval, QRS complex, R-wave progression, ST segment, T waves, and QT/QTc. The safest approach is to use the same sequence every time so that you do not miss important abnormalities.
Introduction
Learning how to read a 12-lead ECG is one of the most important clinical skills in medicine. For medical students, it can feel overwhelming because every tracing seems full of lines, spikes, intervals, and patterns that look almost identical at first glance. For junior doctors, the challenge is often different: you may know the theory, but in real clinical practice you need a fast, repeatable system that helps you interpret the tracing safely under pressure.
The good news is that ECG interpretation becomes much easier once you stop seeing it as a random pattern and start reading it in the same order every time. A 12-lead ECG is not just a rhythm strip. It is a structured recording of the heart’s electrical activity from multiple angles. If you interpret it systematically, you can identify common abnormalities in heart rate, rhythm, conduction, chamber enlargement, ischemia, infarction, electrolyte disturbance, and more.
This guide is written in a mixed educational style for broader traffic, but it is especially designed for medical students and junior doctors who want a practical method they can use on the ward, in clinic, in exams, and in emergency settings.
What Does a 12-Lead ECG Actually Show?
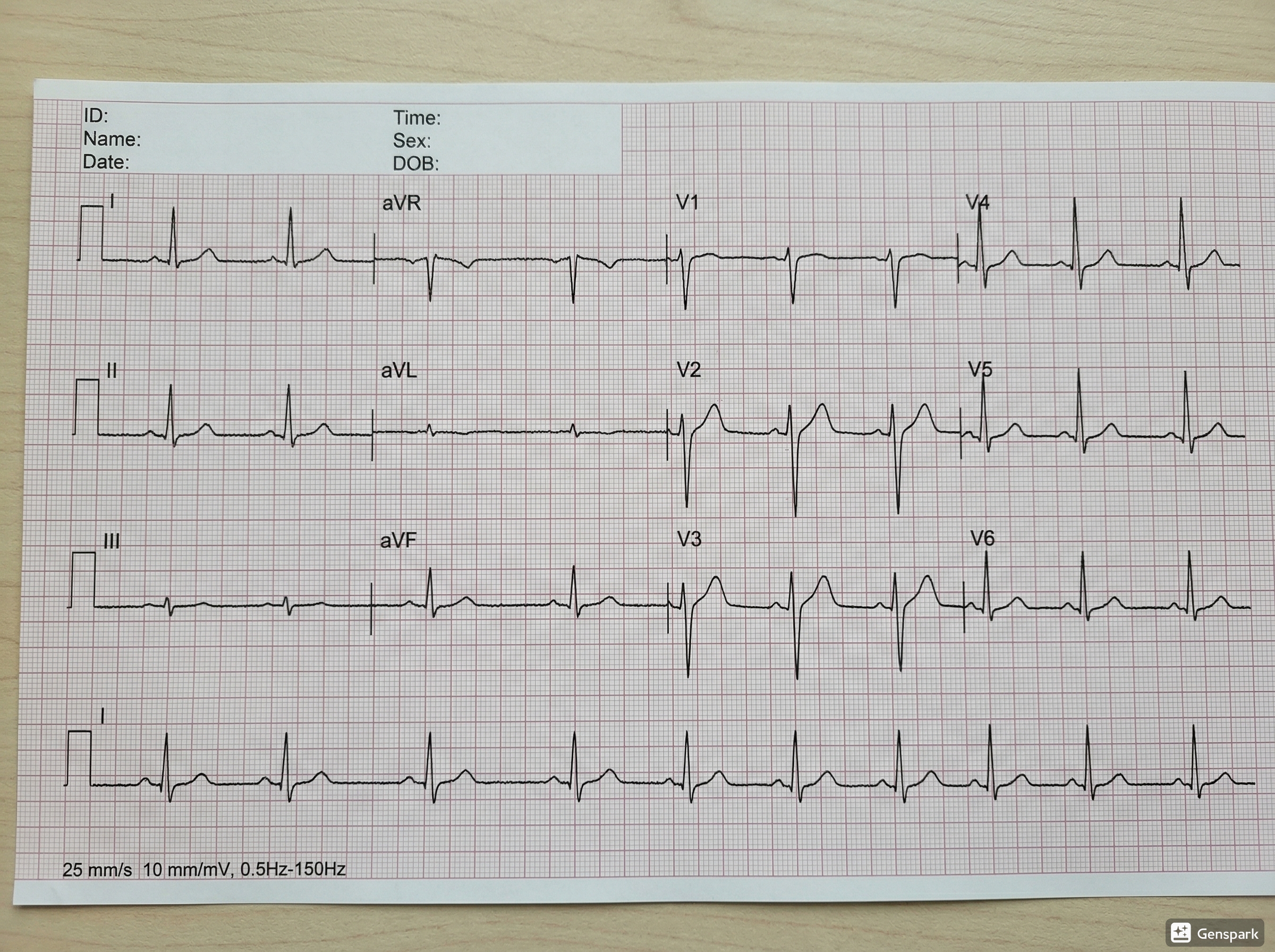
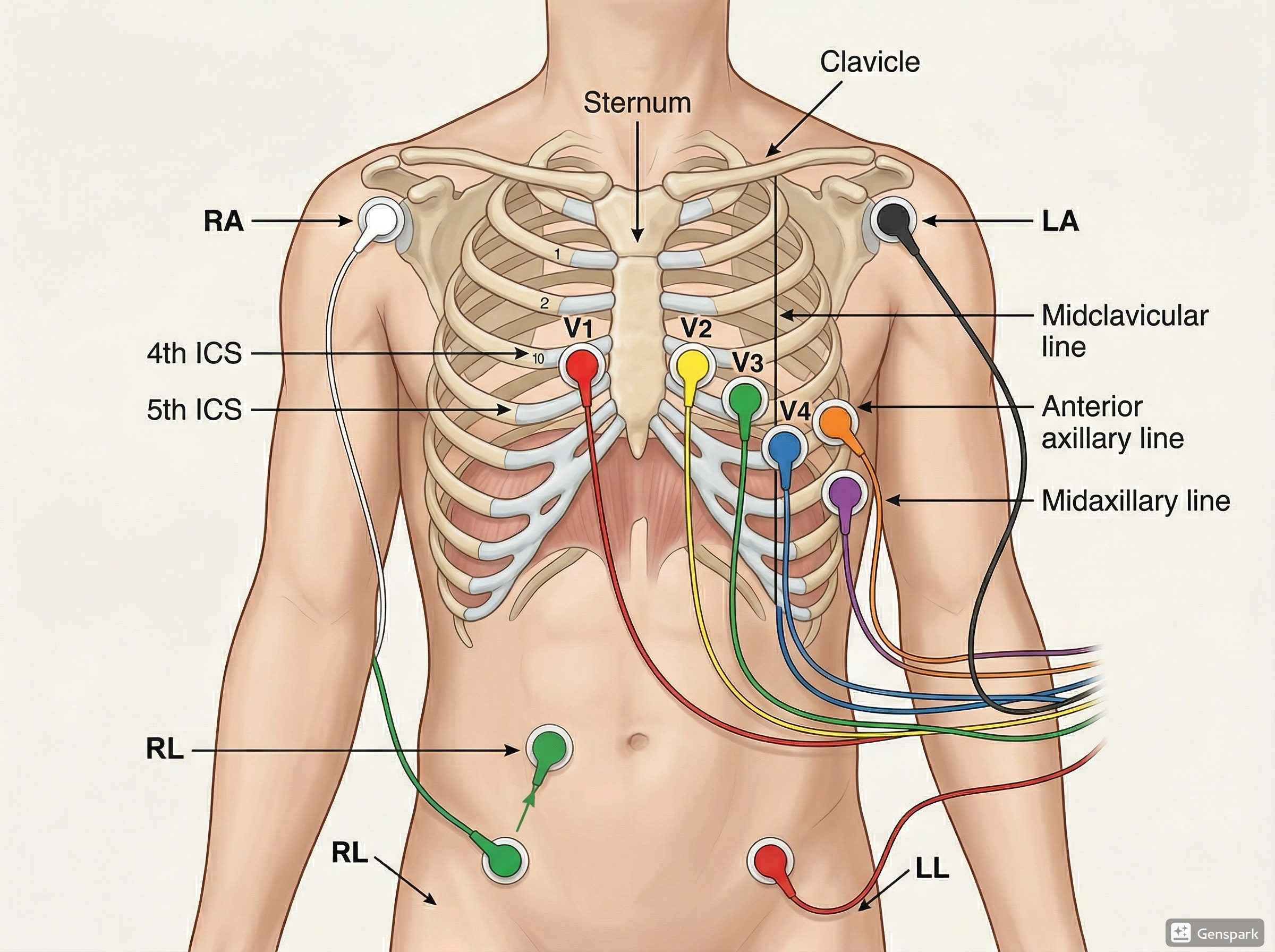
A 12-lead ECG records the electrical activity of the heart from 12 viewpoints. These views are created from 6 limb leads — I, II, III, aVR, aVL, aVF — and 6 chest leads — V1 to V6.
Although we call it a 12-lead ECG, it does not mean 12 separate wires are attached to the patient. The standard setup uses limb electrodes and chest electrodes to generate these 12 perspectives.
The limb leads mainly help you assess the heart in the frontal plane, while the chest leads show the horizontal plane. Together, they allow you to localize abnormalities more accurately. This is why a 12-lead ECG can detect much more than a single rhythm strip.
Before You Start: Confirm the Basics
Before interpreting the tracing itself, always begin with the basics. Check the patient name, date, and time. Make sure you are looking at the correct ECG.
Then check whether the tracing is technically usable. A normal ECG is usually recorded at a paper speed of 25 mm/second and a calibration of 10 mm/mV.
Also look for artifact, loose leads, muscle tremor, or baseline wander. A poor-quality ECG can mimic arrhythmia or ischemia and lead to false conclusions. This first step seems simple, but it prevents avoidable mistakes.
Step 1: Check Calibration and Paper Speed
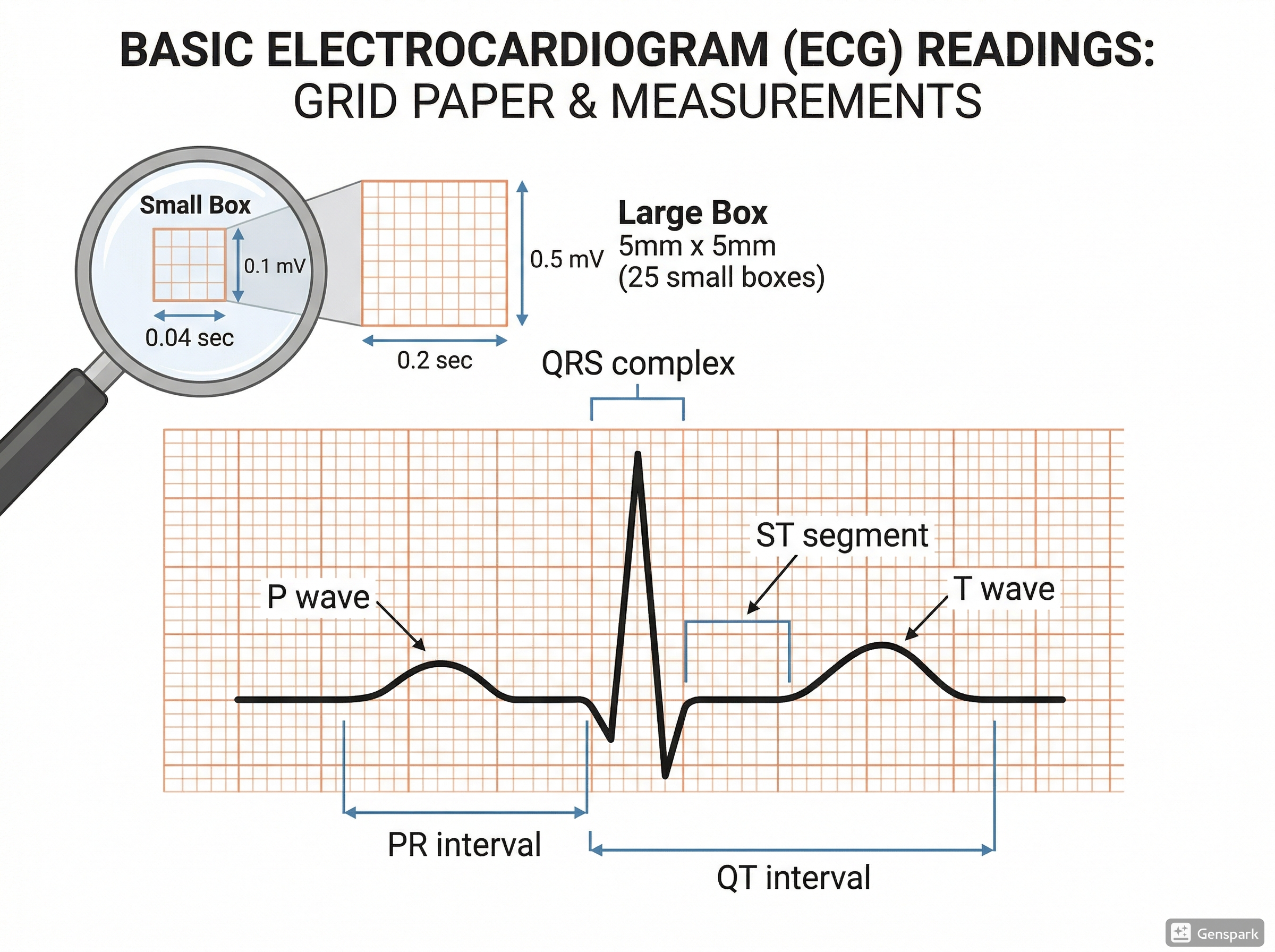
ECG paper is designed to make measurements easier. At standard settings, 1 small square equals 0.04 seconds, 1 large square equals 0.20 seconds, and 5 large squares equal 1 second. Vertically, 10 mm equals 1 mV.
This matters because every interval you measure depends on these assumptions. If you do not confirm the paper speed and gain, your calculations may be wrong. A good beginner habit is to glance at the calibration mark before doing anything else.
Step 2: Calculate the Heart Rate
Once the tracing quality is acceptable, estimate the heart rate.
If the rhythm is regular
Use the 300 rule: 300 divided by the number of large squares between R waves.
- 1 large square = 300 bpm
- 2 large squares = 150 bpm
- 3 large squares = 100 bpm
- 4 large squares = 75 bpm
- 5 large squares = 60 bpm
- 6 large squares = 50 bpm
If the rhythm is irregular
Count the number of QRS complexes in a 10-second strip and multiply by 6. In adults, a normal resting heart rate is usually 60 to 100 bpm, although clinical context matters.
Step 3: Assess the Rhythm
Now ask: Is the rhythm regular or irregular? Look at the R-R intervals. If they are evenly spaced, the rhythm is regular. If they vary, the rhythm is irregular.
Then ask the most important rhythm question: Is there a P wave before every QRS, and is every QRS preceded by an appropriate P wave? If yes, and the P wave morphology is consistent, you are likely dealing with sinus rhythm.
Features of normal sinus rhythm include
- Rate usually 60 to 100 bpm
- Regular rhythm
- Upright P waves in lead II
- Each P wave followed by a QRS
- Constant PR interval
If the rhythm is irregular, think about common causes such as atrial fibrillation, atrial flutter with variable block, ectopic beats, or sinus arrhythmia. A safer habit is to first describe what you actually see before naming the rhythm.
Step 4: Determine the Cardiac Axis
Axis tells you the overall direction of ventricular depolarization in the frontal plane. A simple beginner method is to look at lead I and lead aVF.
- Lead I positive, aVF positive = normal axis
- Lead I positive, aVF negative = possible left axis deviation
- Lead I negative, aVF positive = right axis deviation
- Lead I negative, aVF negative = extreme axis deviation
In many healthy adults, the normal axis is roughly between -30° and +90°. Axis is especially useful when evaluating fascicular blocks, ventricular hypertrophy, chronic lung disease, congenital abnormalities, and wide-complex rhythms.
Step 5: Examine the P Waves
P waves represent atrial depolarization. Ask whether P waves are present, upright in lead II, and whether there is one P wave for each QRS. Also look for abnormal size, width, inversion, or absence.
Important normal points include a P-wave duration usually less than 120 ms and an amplitude usually less than 2.5 mm in inferior leads. Abnormal P-wave findings may suggest atrial enlargement, ectopic atrial rhythm, junctional rhythm, atrial fibrillation, or atrial flutter.
Step 6: Measure the PR Interval
The PR interval reflects conduction from the atria through the AV node into the ventricles. A normal PR interval is typically 120 to 200 ms, which equals 3 to 5 small squares.
A prolonged PR interval suggests first-degree AV block. A short PR interval may be seen in pre-excitation syndromes or junctional rhythms, depending on the context. Measure it rather than estimating it casually.
Step 7: Assess the QRS Complex
Examine whether the QRS is narrow or wide, whether pathologic Q waves are present, whether the voltage is unusually high or low, and whether R-wave progression is normal in the chest leads.
A normal QRS duration is usually less than 120 ms. A narrow QRS usually means ventricular activation is occurring through the normal His-Purkinje system. A wide QRS may suggest bundle branch block, ventricular rhythm, paced rhythm, hyperkalemia, or pre-excitation.
Also assess for pathologic Q waves and poor R-wave progression, which may be caused by infarction, lead misplacement, left ventricular hypertrophy, or normal variation.
Step 8: Look at the ST Segment
The ST segment is one of the most clinically important parts of the ECG. Ask whether it is elevated or depressed, what the morphology looks like, and whether the changes are present in contiguous leads.
ST-segment abnormalities may indicate acute myocardial ischemia or infarction, pericarditis, early repolarization, ventricular hypertrophy with strain, bundle branch block, or electrolyte disturbance. Always interpret ST changes in context rather than in isolation.
Step 9: Assess the T Waves
T waves represent ventricular repolarization. Look for inversion, tall peaked morphology, flattening, biphasic appearance, or abnormal symmetry.
T-wave abnormalities can occur in ischemia, infarction, electrolyte disorders, central nervous system events, bundle branch block, and ventricular hypertrophy. T waves should be interpreted together with the QRS and ST segment.
Step 10: Check the QT and QTc
The QT interval reflects the time from ventricular depolarization to repolarization. Because the QT interval changes with heart rate, clinicians usually focus on the corrected QT, or QTc.
A practical rule for beginners is that QTc is often considered prolonged if it is over about 440 ms in men and over about 460 ms in women. Marked QT prolongation raises concern for malignant ventricular arrhythmias, especially torsades de pointes.
Step 11: Look at the ECG as a Whole
Step back and ask whether the ECG fits the clinical picture. Is there evidence of ischemia, conduction abnormality, chamber enlargement, hypertrophy, or anything acute or dangerous? Is there an older ECG for comparison?
A tracing is never interpreted in isolation. A borderline ECG in a well outpatient means something different from the same tracing in a hypotensive patient with chest pain. Comparing with prior ECGs is one of the most useful and underused habits in real practice.
A Simple ECG Interpretation Sequence to Memorize
Calibration → Rate → Rhythm → Axis → P waves → PR interval → QRS → ST segment → T waves → QTc → Clinical context
If you repeat that order on every ECG, your confidence and speed will improve dramatically.
Common Beginner Mistakes
One common mistake is skipping straight to ST elevation or T-wave inversion before checking rate, rhythm, and QRS morphology. Another is forgetting to confirm calibration and paper speed. Many learners also overdiagnose pathology in tracings that are actually normal variants or distorted by artifact.
Another frequent problem is trying to memorize hundreds of patterns before mastering the basics. In reality, most good ECG readers are using a disciplined routine rather than magic pattern recognition alone.
Practical Example of a Normal ECG Approach
Imagine you are handed a normal ECG. You first confirm the patient details and calibration. The rate is about 75 bpm. The rhythm is regular. There is one upright P wave in lead II before every QRS. The PR interval is normal. The QRS is narrow. Axis is normal. R-wave progression across the precordial leads looks appropriate. There is no significant ST elevation or depression. T waves are normal for the lead distribution. QTc is within normal limits.
That is exactly how you should present it: “Normal sinus rhythm at 75 bpm, normal axis, normal intervals, no acute ischemic changes.” This kind of structured conclusion sounds clear, professional, and safe.
FAQ
What is the easiest way to read a 12-lead ECG?
The easiest way is to use the same order every time: calibration, rate, rhythm, axis, P waves, PR, QRS, ST segment, T waves, QTc, and clinical context.
What is normal sinus rhythm on ECG?
Normal sinus rhythm usually means a regular rhythm between 60 and 100 bpm, upright P waves in lead II, one P wave before each QRS, and a constant PR interval.
What is a normal PR interval?
A normal PR interval is typically 120 to 200 milliseconds, or 3 to 5 small squares.
What is a normal QRS duration?
A normal QRS duration is usually less than 120 milliseconds.
Why is a 12-lead ECG better than a rhythm strip?
A rhythm strip mainly helps with rhythm analysis, but a 12-lead ECG shows the heart’s electrical activity from multiple angles and can help identify ischemia, infarction, axis deviation, hypertrophy, and conduction abnormalities.
Key Takeaways
Reading a 12-lead ECG becomes much easier when you stop trying to guess the diagnosis from the first few seconds and instead use a fixed, repeatable sequence. Start with the technical basics, then work through rate, rhythm, axis, atrial activity, AV conduction, ventricular conduction, repolarization, and finally the clinical context.
For medical students and junior doctors, the best long-term strategy is not to memorize isolated patterns first. It is to practice a structured interpretation method until it becomes automatic. Once that foundation is strong, abnormal ECGs become much easier to recognize.
References
- American Heart Association. Electrocardiogram (EKG or ECG).
- National Heart, Lung, and Blood Institute. Heart Tests.
- ECG Waves. How to Interpret the ECG: A Systematic Approach.
- ECG Waves. Characteristics of the Normal ECG.
- LITFL. ECG Basics.
- LITFL. Normal Sinus Rhythm.
- LITFL. PR Interval.
- LITFL. QRS Interval.