Common ECG Artifacts and How Not to Misread Them
Description: Learn the most common ECG artifacts, including baseline wander, muscle tremor, AC interference, and lead misplacement, and how to avoid mistaking them for real pathology.

Quick Answer
Common ECG artifacts include baseline wander, muscle tremor artifact, AC interference, electrode noise, and lead misplacement or lead reversal. These patterns can mimic arrhythmia, ischemia, infarction, chamber enlargement, or axis deviation if you do not recognize them. The safest approach is to check the patient, the leads, and the overall plausibility of the tracing before calling an abnormality real.
Introduction
One of the easiest ways to make a wrong ECG diagnosis is to trust a bad tracing. ECGs are powerful because they can reveal heart rate, rhythm, conduction abnormalities, ischemia, infarction, and much more. But they are also vulnerable to artifact. If the signal quality is poor, the tracing may look dramatic while the patient is completely stable, or it may falsely suggest dangerous pathology that is not actually there.
For medical students and junior doctors, artifact recognition is a core safety skill. You do not need to become an electrophysiology expert to avoid the most common mistakes. You need a systematic habit: ask whether the tracing makes physiological sense, check whether the abnormality appears in all leads or only some of them, and think about whether a technical issue could explain what you are seeing.
This article explains the most common ECG artifacts, why they happen, how they can fool you, and how to avoid misreading them in clinical practice.
What Is an ECG Artifact?
An ECG artifact is any distortion on the tracing that does not truly represent the patient’s cardiac electrical activity. Artifact may come from patient movement, poor electrode contact, muscle activity, external electrical interference, or incorrect lead placement. Some artifacts merely make the tracing messy. Others can imitate major pathology such as atrial fibrillation, ventricular tachycardia, bundle branch block, or myocardial infarction.
This is why artifact matters. It is not just an aesthetic problem. It can lead to misdiagnosis, unnecessary tests, inappropriate treatment, and avoidable anxiety for both clinicians and patients.
A Simple First Question: Does the ECG Fit the Patient?
Before analyzing any unusual tracing, ask whether it matches the clinical picture. If a patient is awake, comfortable, talking normally, and has a monitor pulse of 75 bpm, a rhythm strip that appears to show an unstable wide-complex tachycardia should immediately make you consider artifact. The tracing never exists in isolation. Always compare the ECG appearance with the patient, the pulse, and the monitor data if available.
Common ECG Artifact Types
1. Baseline wander
Baseline wander is a slow drifting up-and-down movement of the ECG baseline. It commonly occurs because of respiration, body movement, loose electrodes, perspiration, or dry electrodes. Even a small amount of baseline wander can make ST segments and T waves harder to judge accurately, which is why it is especially important in chest pain assessment.
Baseline wander usually looks like the whole tracing is floating or moving gently across the page rather than staying fixed on a stable baseline.
2. Muscle tremor artifact
Muscle tremor artifact produces rapid irregular noise on the tracing. It may be caused by shivering, anxiety, tension, Parkinsonian tremor, or patient movement. This artifact can create a chaotic appearance and may be mistaken for atrial fibrillation, flutter, or other tachyarrhythmias if the underlying QRS complexes are not identified carefully.
3. AC interference
AC interference, also called power-line interference, produces a repetitive regular electrical noise pattern. It is often related to nearby electrical devices, poor grounding, or signal contamination. Unlike muscle tremor, which is usually irregular and jagged, AC interference tends to be more uniform and repetitive.
4. Electrode noise and poor contact
If an electrode is loose, dry, expired, placed on oily skin, or applied over hair without adequate preparation, the signal may become unstable. This can produce intermittent distortion, baseline shifts, or noisy segments that make interpretation unreliable.
5. Lead misplacement and lead reversal
Lead misplacement is not just a technical nuisance. It can create pseudo-pathology. Limb lead reversal may mimic ectopic atrial rhythm, chamber enlargement, ischemia, infarction, dextrocardia, or axis deviation. Misplaced chest leads, especially V1 and V2 placed too high, may create false patterns that resemble anterior ischemia, right bundle branch block, or anterior T-wave inversion.
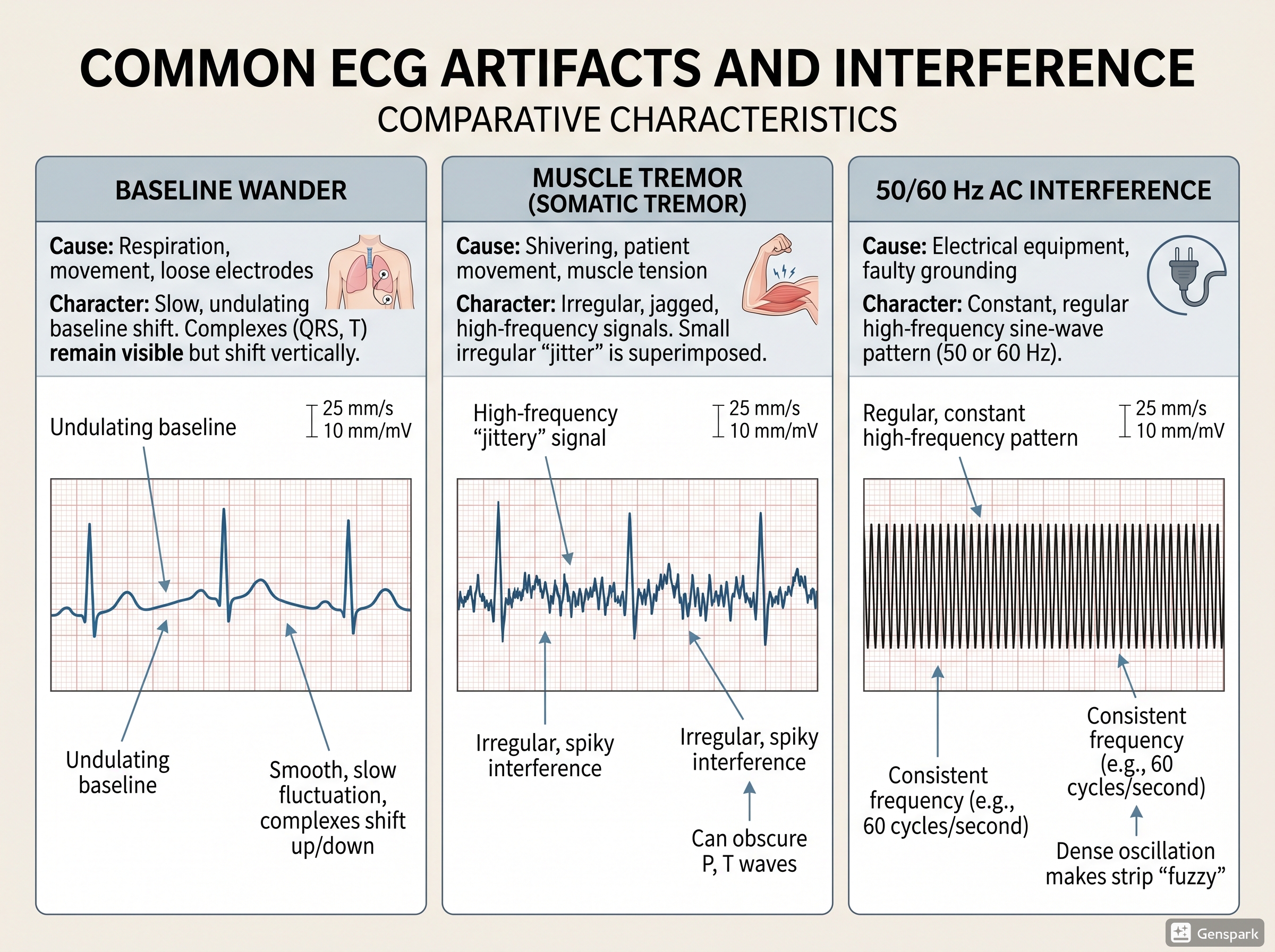
Baseline Wander: How Not to Misread It
Baseline wander is especially dangerous when you are looking at the ST segment. If the baseline is drifting, small apparent ST elevations or depressions may not be real. Beginners sometimes overcall ischemia because they measure from a moving baseline rather than a stable one.
Clues that favor baseline wander include gradual undulation of the whole tracing, varying baseline position from moment to moment, and otherwise preserved recognizable QRS complexes. If you suspect baseline wander, check lead contact, ask the patient to keep still, dry the skin if needed, and repeat the ECG.
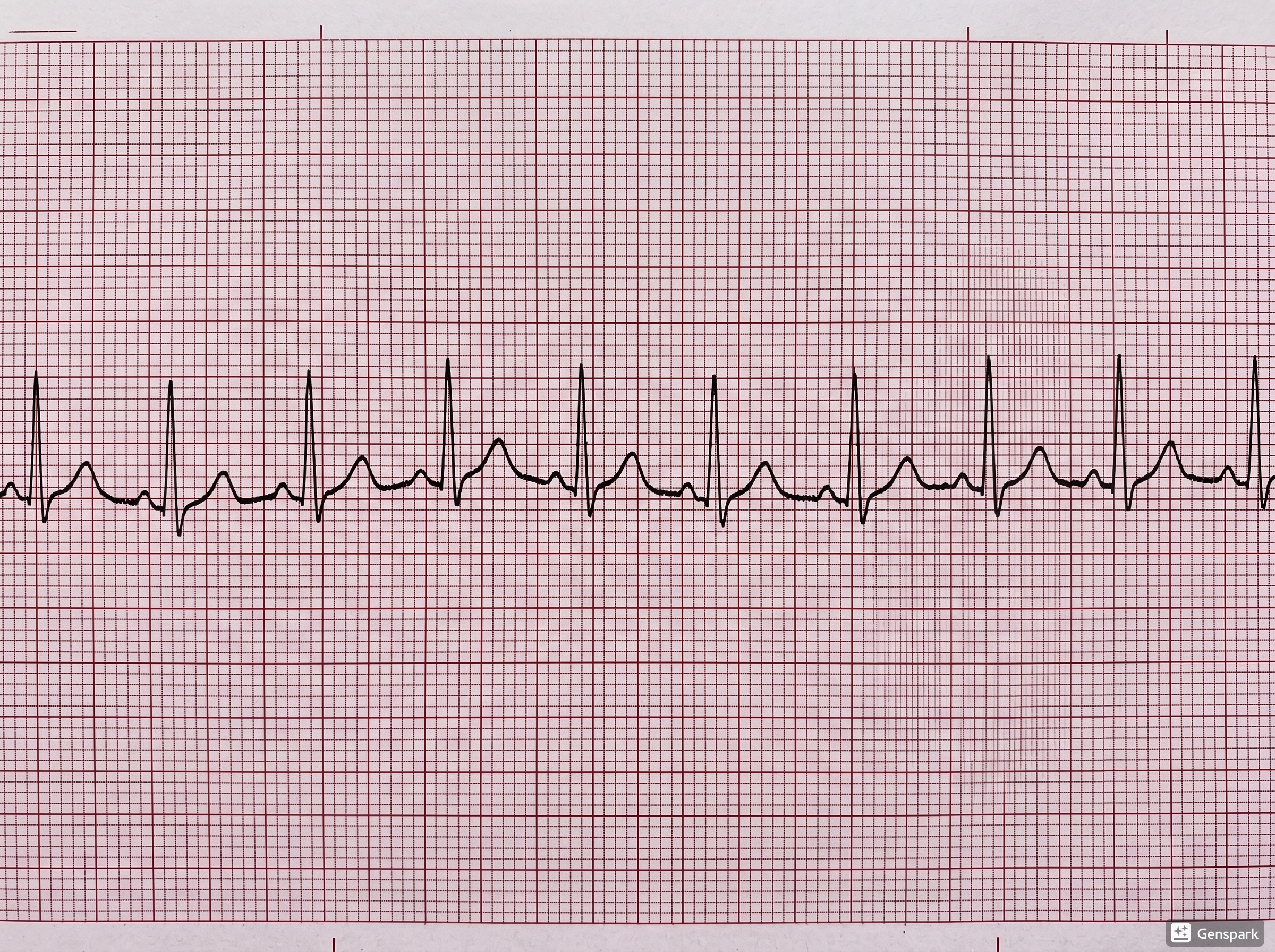
Muscle Tremor Artifact: Why It Mimics Arrhythmia
Muscle tremor artifact can create a very busy tracing that makes the rhythm look fast or chaotic. The key mistake is focusing on the noise rather than finding the real QRS complexes. If the QRS complexes march through at a consistent rate beneath the noise, the patient may have a normal or relatively stable rhythm despite the dramatic appearance.
Clues that favor muscle artifact include high-frequency jagged distortion, inconsistent noise amplitude, and preservation of an underlying rhythm when you look carefully. If the patient is shivering, anxious, or moving, the diagnosis becomes even more likely.
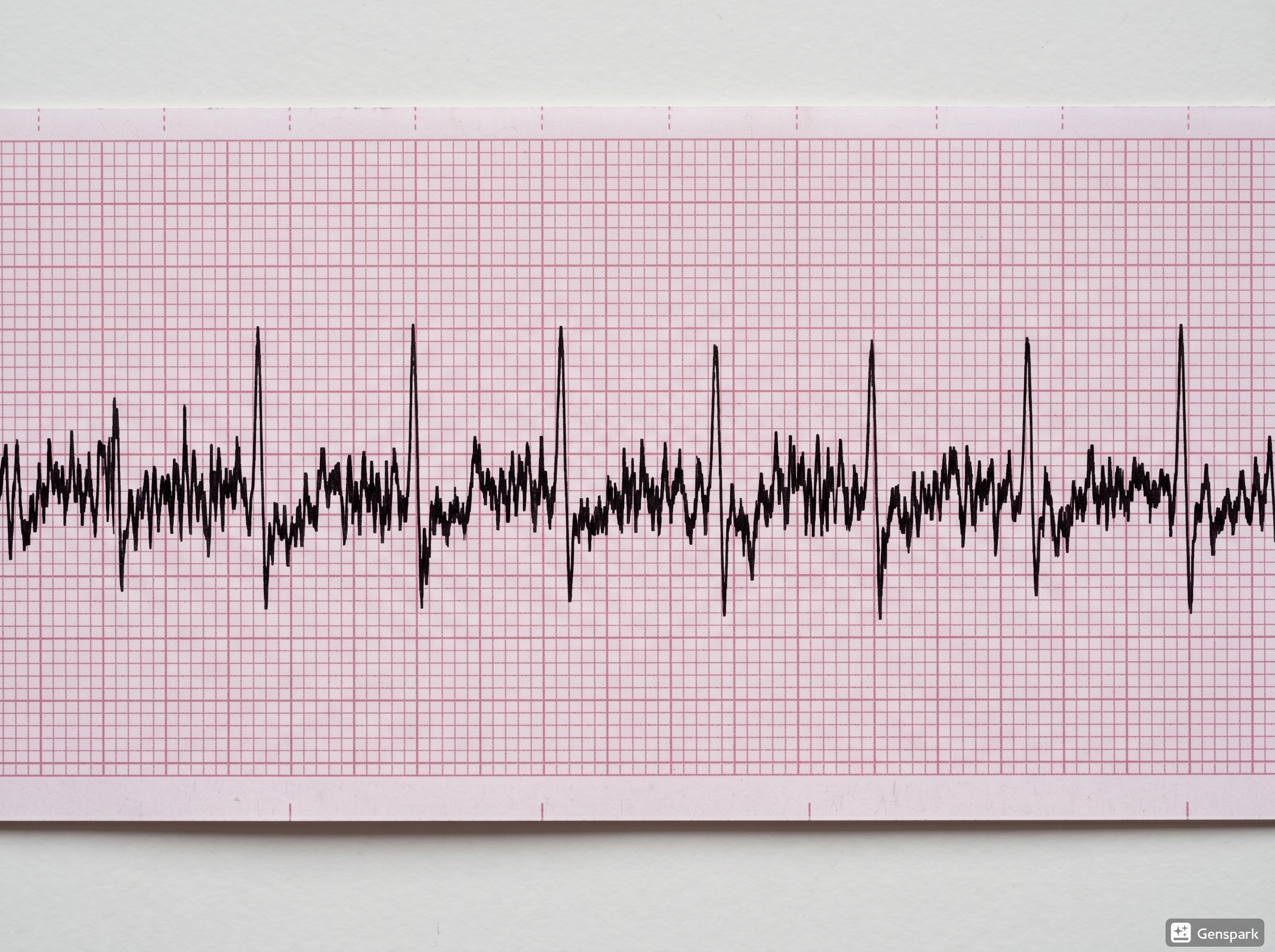
AC Interference: The Regular Artificial Noise Pattern
AC interference tends to look more repetitive and uniform than muscle tremor artifact. It can make the ECG appear electrically “busy” without truly changing the patient’s cardiac rhythm. Turning off nearby interfering devices, improving grounding, and checking the ECG environment can help resolve it. In practice, if the noise looks mechanically repetitive rather than physiologically irregular, think about external interference.
Lead Misplacement: A Major Source of Pseudo-Diagnosis
Lead misplacement is one of the most important causes of misleading ECGs. It does not merely reduce quality; it can produce a convincing but false abnormal pattern. This is why you should be cautious whenever the ECG appears surprising, inconsistent with the patient, or incompatible with previous tracings.
Misplacement of V1 and V2 too high on the chest is especially common. This may create patterns that resemble right bundle branch block, anterior ST-segment abnormalities, or anterior T-wave inversion. If the tracing looks strange in the anterior leads, always ask whether the precordial leads were placed correctly.
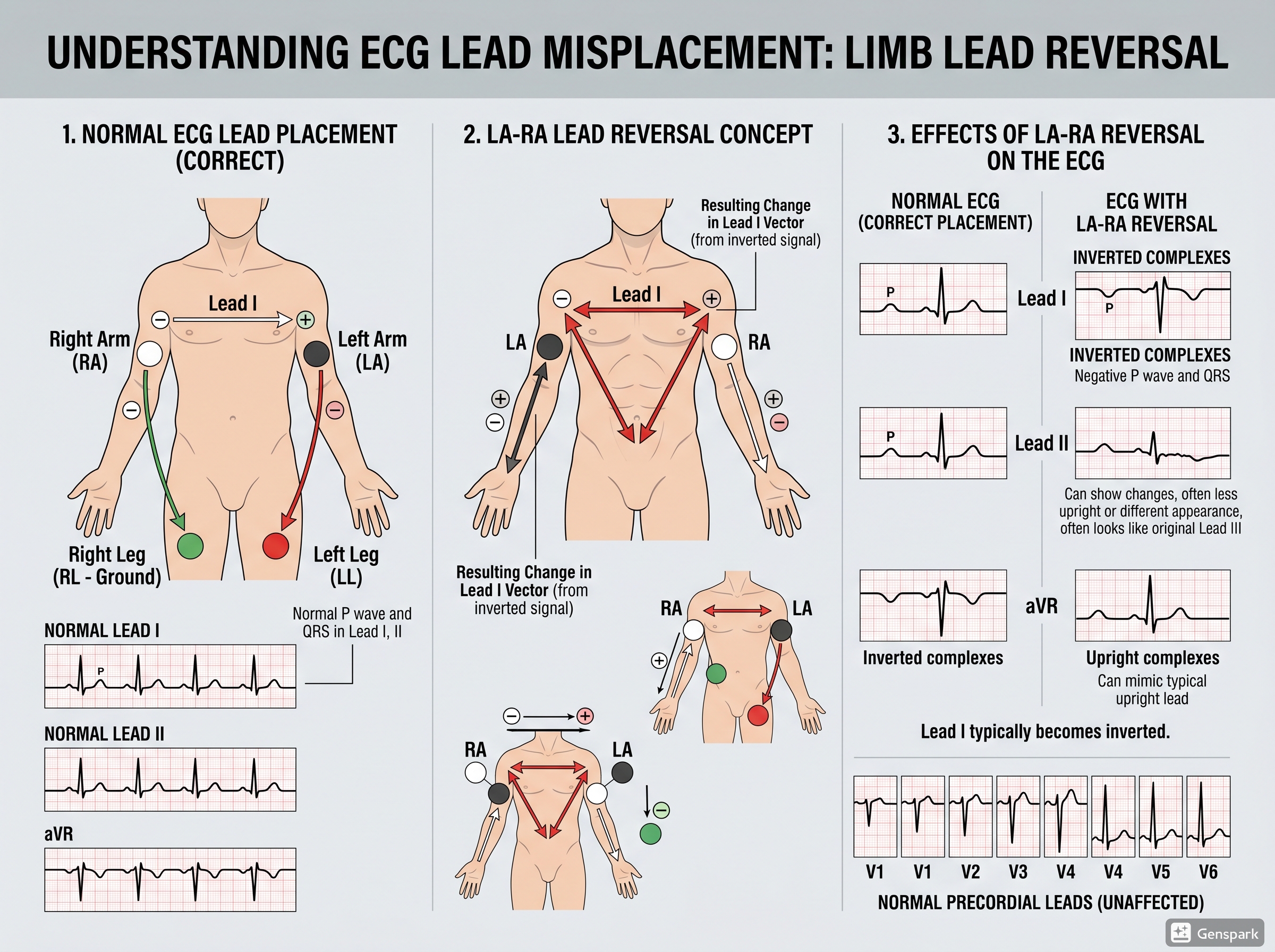
Limb Lead Reversal: The Classic Artifact That Mimics Disease
Limb lead reversal is a classic teaching point because it can simulate important pathology. One of the most common patterns is left arm-right arm reversal. In this situation, lead I becomes inverted, leads II and III switch places, aVL and aVR switch places, and aVF remains unchanged.
A quick bedside clue for left arm-right arm reversal is this: if lead I is completely inverted and aVR looks unexpectedly positive, think about lead reversal before diagnosing a major axis abnormality or dextrocardia. In true dextrocardia, the precordial lead progression is also abnormal, whereas in simple limb lead reversal the precordial R-wave progression remains normal.
How to Avoid Misreading Artifact as Pathology
- Look at the patient first. Does the ECG match the clinical picture?
- Check whether the apparent abnormality is seen consistently across appropriate leads.
- Search for a stable underlying QRS rhythm beneath noisy segments.
- Be suspicious of bizarre axis changes or inverted lead I if lead reversal is possible.
- If the tracing is poor, repeat the ECG after correcting technical issues.
- Compare with an older ECG whenever available.
These small habits prevent many misinterpretations. The safest clinician is not the one who calls every strange tracing abnormal, but the one who knows when a tracing may be technically unreliable.
Practical Troubleshooting at the Bedside
- Ask the patient to relax and keep still.
- Warm a shivering patient if possible.
- Clean oily or sweaty skin before electrode application.
- Shave excessive hair if it prevents good contact.
- Replace dry, old, or poorly adherent electrodes.
- Separate and recheck lead cables carefully.
- Repeat the ECG after correcting the problem.
These steps are simple, but they dramatically improve signal quality and reduce diagnostic error.
Common Beginner Mistakes
One common beginner mistake is diagnosing arrhythmia from noise alone without identifying the true QRS complexes. Another is calling ST elevation on a tracing with obvious baseline drift. A third is forgetting that lead reversal can mimic real disease very convincingly.
Students also sometimes assume that if the machine printed an interpretation, the tracing must be technically reliable. That is not safe. ECG machines can be fooled by bad signal quality just as humans can.
A Simple Safety Rule
If the ECG looks dramatic but the patient looks well, pause and think artifact. That does not mean ignore the tracing. It means confirm it. Check the leads, assess the pulse, repeat the ECG, and only then decide whether the pattern is real.
FAQ
What is the most common ECG artifact?
Common ECG artifacts include baseline wander, muscle tremor artifact, AC interference, and lead misplacement. The exact “most common” artifact varies by setting and patient factors.
Can ECG artifact look like atrial fibrillation?
Yes. Muscle tremor artifact can create a chaotic tracing that may be mistaken for atrial fibrillation if the underlying QRS complexes are not identified carefully.
Can lead reversal mimic myocardial infarction?
Yes. Limb lead reversal can mimic ischemia, infarction, axis deviation, or dextrocardia. Always consider technical error when the ECG does not fit the patient.
How do you recognize baseline wander?
Baseline wander usually appears as slow drifting movement of the ECG baseline, often caused by respiration, loose electrodes, perspiration, or patient motion.
What should you do if the ECG looks noisy?
Check the patient, improve skin preparation, replace poorly adherent electrodes, correct lead placement, reduce motion if possible, and repeat the ECG before making major decisions from a poor-quality tracing.
Key Takeaways
Common ECG artifacts can mimic serious pathology, including arrhythmia, ischemia, infarction, and abnormal axis. The most important examples are baseline wander, muscle tremor artifact, AC interference, poor electrode contact, and lead misplacement or reversal.
For medical students and junior doctors, the safest approach is simple: look at the patient, question whether the tracing is technically reliable, and repeat the ECG when necessary. Recognizing artifact is not a minor skill. It is part of accurate, responsible ECG interpretation.
References
- American Heart Association. Electrocardiogram (EKG or ECG).
- LITFL. ECG Limb Lead Reversal.
- LITFL. Lead Reversal: Left Arm/Right Arm.
- GE HealthCare. ECG Signal Quality: A Practical Guide for ECG Readings.
- GE HealthCare. ECG Lead Misplacement: Looking at Common Issues.